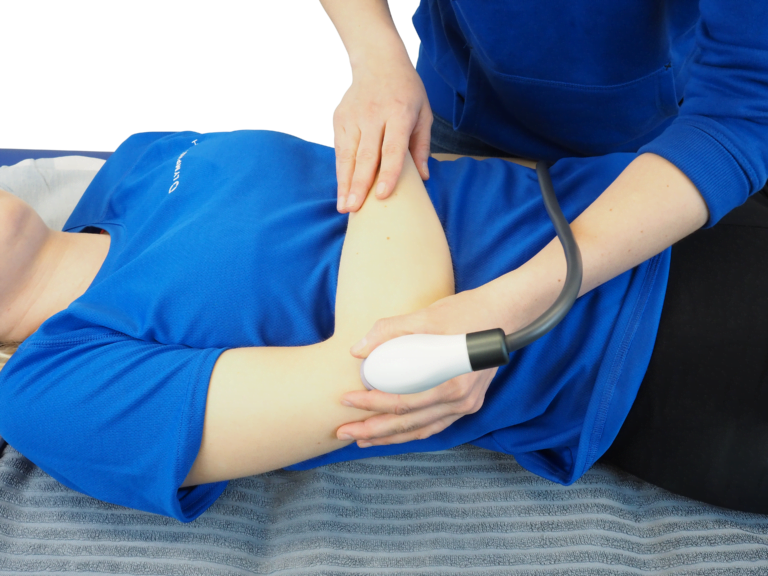
Background
I have used LymphTouch in the clinic with patients with secondary Lymphoedema. It quickly softened forearm fibrosis and softening and improved symptoms maintained for several weeks in patients concordant with hosiery wear.
I was curious about whether the device could also achieve softening in tissues that are chronically fibrosed and which appear to be resistant to the effects of compression bandaging as part of DLT (decongestive lymphatic therapy). I am an advocate of using different modalities in combination when treating Lymphoedema. This case study demonstrates that introducing different technologies and techniques together can achieve better results than always using the same approach.
Lymphoedema patient:
Female, 67yrs old, Borderline type 2 diabetes & IBS. Ca Uterus 2016 yrs ago, which was treated surgically with a total abdominal hysterectomy and lymph node clearance. Postoperative complications of delayed wound healing and subsequent Lymphoedema to the abdominal apron.
High BMI. Weight:143kg. Ambulant, but now unable to find footwear suitable for outdoors. Fully concordant in daily skincare and hosiery wear.
Diagnosed in 2000, referred to local Lymphoedema Service where she has received care since. This has included: intermittent pneumatic compression, DLT, MLD, Kinesiology taping and Class 3 forte custom fit stockings for daily wear. She has not had any active treatment in the clinic since March 2018 but her clinic oversees 6-12 monthly reviews of hosiery. Since the COVID19 pandemic, she has had 1 recent telephone review with no changes proposed.
Since 2018, she has been receiving weekly treatments from First LymphCare, because she was concerned that the symptoms of heaviness and discomfort in her Lymphoedematous legs was increasingly problematic.
Lymphoedema Staging: Severe, chronic. (longstanding symptoms of several years) to both lower legs and feet. Right leg more affected than the left leg.

Chronic Bilateral Lymphoedema. Copyright Sue Hansard, First LymphCare.
Note: There is currently no formal system for the classification of the severity of bilateral limb swelling. Skin condition, tissue texture, stemmers sign, presence of secondary changes to both skin and tissues, papillomatosis, hyperkeratosis, blanching, limb shape/shape distortion, skin folds, nailbed changes, plantar oedema, are all taken into account in assessment (ref: International Lymphoedema Framework, 2016).
Presentation
Severe chronic swelling to Dorsii and lower legs and plantar aspect of feet. Skin intact and well moisturised. Deep skin fold to right lateral/ankle achilles region. Shape distortion to R foot and digits, with papillomatosis to digits. Right leg and foot are more swollen than the left.
Positive stemmers sign. Gaiter areas are slightly pink, with no sign of infection. The tissue’s firm, with no pitting from the dorsum to the popliteal fossa. Medial lower thigh fibrotic tissue/overhang, R > L.
Upper legs tissues are soft and the abdominal apron is now soft too.

Photo 1: Pre Treatment. Copyright Sue Hansard, First LymphCare.
Current management
- Skincare: The patient is concordant in all aspects of skincare, infection prevention and compression wear. Weight management is a complex life long issue.
- Compression: CLASS 3 FORTE. JOBST custom fit, below the knee, closed-toe garments daily for 12 hours. Wears old garments at night.
- She sometimes also uses the Juzo Velcro Wrap system on top of compression stockings.
- Active treatments: Weekly deep oscillation and massage prior to lockdown.

Day 1: Pretreatment with LymphaTouch. Copyright Sue Hansard, First LymphCare.
Plan after lockdown
- Decongestive Lymphatic Therapy: Lymph drainage using LymphaTouch to right leg, for 6 weekly treatments.
AIM – To empty lymph nodes, improve lymph flow and encourage a loosening of fibrotic tissue, and improved circulation. - Coban 2 bandaging. Applied weekly for 4 weekly applications.
AIM – To reduce volume, increase lymph flow, soften tissues. - New Class 3 garments, daytime.
AIM – To maintain lymph and venous return and limit rebound effect and firming up of tissues. - Thuasne Modiberm custom fit padded garment nightly or alternate nights.
AIM – To maintain softening and improve symptoms of heaviness and solidity in tissues.
Lymphatouch sequence (week 1 – 30 minute session)
- QV moisturiser was used to facilitate gliding action of cup over skin.
- CUP SIZE: 60mm. Right Inguinal nodes, right popliteal nodes (100mmHg).
- CUP SIZE: 60mm. Lower leg, anterior and posterior aspects (140-160mmHg).
- Gliding movement with twisting action and intermittent pulse draining towards popliteals (20 minutes).
- CUP SIZE: 35mm. Skin fold over achilles. This tissue forms a hard, non moveable cuff (80-100mmHg).
- CUP SIZE: 50mm and 2 to dorsum and plantar aspect of foot.
- CUP SIZE: 10mm to great and second toes, where there are papillomatosis (60-80mmHg).
“During treatment patient reported that the treatment felt comfortable.”
The clinician noted that the calf was beginning to soften and superficial softening was noted to dorsum and skin fold edges.
After skin moisturisation, compression bandages were applied: including toe bandages, Compression was from the base of toes to just below the knee. The patient would remove bandages on day 4 for hygiene needs and revert to usual compression stockings and Juzo ACS wrap.
(Ideally, Coban 2 layer compression should be reapplied x 2 weeks, but this is costly when self-funding. The patient requested x 1 week instead).

After week 1 of DLT. Copyright Sue Hansard, First LymphCare.
Week 2
- Tissues visibly softer.
- Dimples show the effect after 20 minutes (Mobiderm garment)
- Less resistance in calf and Achilles area, wrinkling to superficial tissues of the dorsum
- The patient and clinician agreed that the changes were greater than those achieved with previous DLT treatments and the patient reported that the calf area felt tender after first treatment therefore 100-120mmHg used this time
The same sequence and cup sizes were used as week 1.
Weeks 3, 4 and 5
- Tissues are softer to the calf and the skin fold, Dorsum beginning to soften superficially
- Limb volumes have re- bounded to pre- bandaging measurements which is the usual pattern for this patient when she reverts to her Class3 hosiery
However, the tissues have stayed softer with less resistance and the patient commented that her legs `feel lighter’ and ‘mobilising is easier with improved comfort during day and night.’
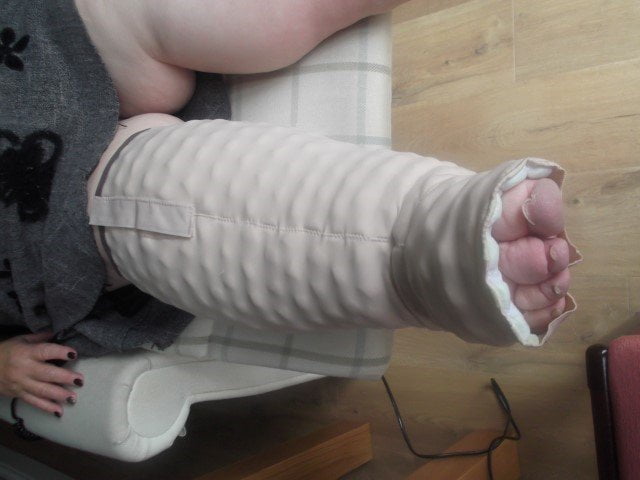
Mobiderm night-time stocking. Copyright Sue Hansard, First LymphCare.
Week 5
Mrs S has managed to wear her Mobiderm garment each night and on examination, the softening of tissues which LymphaTouch and Coban 2 bandaging achieved, has been maintained and even improved.
Mrs S felt as if the leg was smaller because it felt `lighter’ and she had more flexibility within the ankle and knee.
Limb volume measurements showed that the following reductions:
- Skin fold circumference had reduced by 1cm (distally) 2cm (proximally)
- Calf circumferences, reduced by 1cm distally, and 4cm (proximal, upper calf)
- Circumference just below the knee reduced by 3cm
Week 6: Patient feedback
“The combination of day and night time garments is helping to maintain the softening in lower limb tissues which LymphTouch initiated.”
The patient feels that her limb `is lighter, less painful and easier to move’. She feels she has been given hope.
Clinician comments
- Calf tissues remained softer between treatments each week
- As deeper tissues softened, it was necessary to reduce the pressures of the device due to increased, localised sensitivity to the suction effect
- It became easier to glide the cups during treatment as softening occurred
- Using a twist technique helps to release fibrosis
- If LymphTouch was used as part of her weekly treatment I believe it would continue to release the chronically fibrosed tissues, especially in her foot. And this could potentially improve swelling enough to enable her to get better footwear.
- The positive psychological impact that even these small physical changes have made for this patient, is significant. It has given her small hope that at the very least, her lymphoedema can be prevented from getting worse. And also that treatment modalities are constantly being researched and developed, which gives hope and reassurance that people living with life-impacting conditions, are not being forgotten.
Conflict of interest:
There are no conflicts of interest. Physiquipe Loaned LymphaTouch to me for a 2 month trial period. Thuasne have kindly provided the garment for this patient and I have also provided a case study for them. First LymphCare is my independent business.
I am very grateful for the support I had from Physiquipe and Thuasne in my care for Mrs S.
All photographs are by Sue Hansard and are copyright. However, Physiquipe and Thuasne may use them with permission for teaching and promotional work.
Mrs S agreed to trialing LymphaTouch as part of her treatments and has consented to the sharing of this case study and photographs, with Physiquipe and Thuasne so that it can be used for professional learning by Physiquipe, Thuasne and First LymphCare.